[NB: check the byline, thanks. /~Rayne]
** 8:30 PM ET — UPDATE AT THE BOTTOM OF THIS POST. **
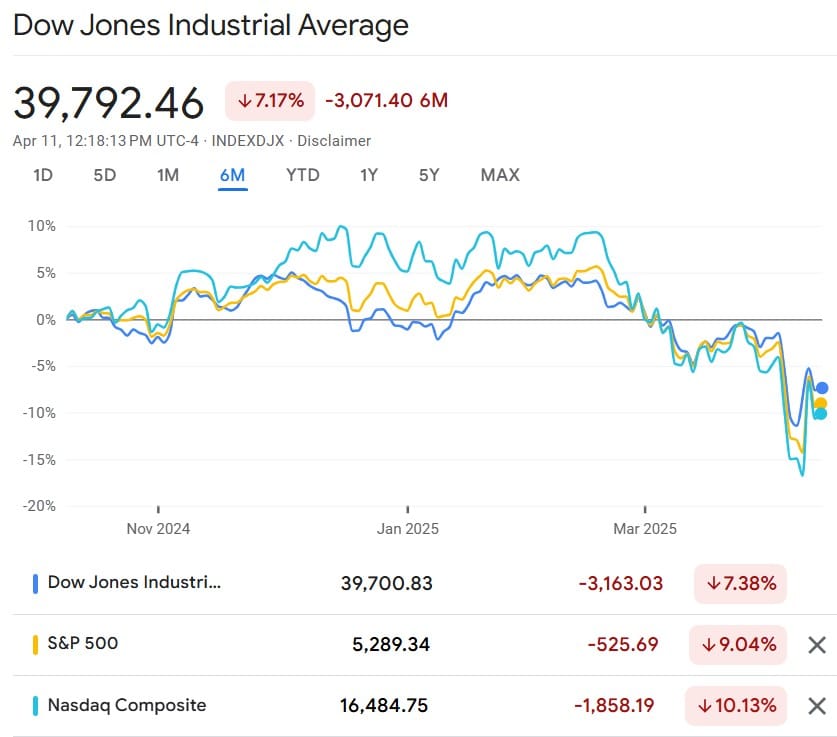
While the market and Americans’ college funds, 401Ks, and retirement accounts whipsawed today after their multi-day plummet, somebody had other priorities.

I don’t know at what time this was published by the White House, but this has Trump’s tiny grip all over it.
He’s obsessed with water pressure, confusing it with showerhead function; he’s been obsessed for years with this.
December 27, 2019 – Trump Vs. Toilets (And Showers, Dishwashers And Lightbulbs)
July 23, 2020 – With 137,000 U.S. Deaths, Trump Stays Focused on Shower Heads
August 13, 2020 – ‘My hair has to be perfect’: Trump prompts change in showerhead rule – video
August 21, 2020 – Trump talks shower heads, sharks, and more on DNC’s last day
December 17, 2020 – Trump Bemoaned Water Pressure. Now His Administration Has Eased Standards
August 6, 2023 – ‘I Want Water To Pour Down On Me’: Trump Has Cold Words For Showers At GOP Dinner
January 7, 2025 – Making Sense of Trump’s January 2025 Remarks About Showerheads and Rain Falling from Heaven
I’m sure if I dig harder I can find more instances where Trump whined about water pressure in the shower but you get the gist.
And like 2020 when Americans were dying by the thousands each week from COVID and Trump complained about showerheads, Trump once again leaned into his personal bête noire while Americans became increasingly panicked about their financial well being and the state of the nation’s economy under Trump’s tariff-tax.
It’s ridiculous that our country has allowed one exceedingly vain man spend so much of our tax dollars on something which will not result in the blast of water he wants for his “perfect” hair.
Musk and his Muskrats are taking a chainsaw to our entire government, creating enormous risks in the misbegotten effort to increase efficiency and cut government spending — and Trump pisses away any efficiencies with his obsessive, unnecessary change to water and energy saving regulations affecting showerheads.
When the next Articles of Impeachment are drafted, there should be an article for abuse of power for personal use with Trump’s fucking obsession with showerheads as an example. Especially since it’s a form of lawmaking by the executive branch to the detriment of the American public.
~ ~ ~
While Trump was dicking around with his bête noire, the House Ways and Means Committee held a hearing. Many of you have already read or heard about Rep. Steven Horsford’s (D, NV-02) questions to U.S. Trade Representative Jamieson Greer about the dramatic change in the Trump administration’s approach to tariffs — a change which was announced over social media by Trump while Greer was in front of the committee, without apparent advance notice to Greer.
As Horsford noted, the Republicans on the committee weren’t in attendance. It’d be nice to know if those weasels left because they didn’t want to be on the spot on camera during the hearing, or if they were daytrading to capitalize on the announcement.
What isn’t being discussed is that the Senate had a similar hearing the day before during which Greer also testified about the tariffs. Senator Thom Tillis (R-NC) didn’t sound too happy with the Trump tariff-tax strategy, asking, “Whose throat do I get to choke if this proves to be wrong?”
Greer does a weaselly tap dance in response.
Sen. Catherine Cortez Masto also grilled Greer more pointedly about the Trump tariff-tax upending the trade agreements including the United States-Mexico-Canada Agreement (USMCA) the Trump administration spent two years working on during Trump’s first term.
She asked, “Why would any country want to do business with us, much less negotiate a trade deal if we don’t even honor our ongoing our ongoing agreements?”
Greer did his weaselly tap dance again and she called him out on this because she and Greer had had a one-on-one discussion in her office about trade matters and the USMCA including a blanket tariff strategy.
It’s hard not to watch these video segments from two days of hearings and not come away thinking Greer’s job has nothing to do with trade and everything to do with providing a punching bag between the Trump tariff-tax and our elected representatives.
He does little in these excerpts to make one feel any better about the Trump tariff-tax, mostly because Trump himself appears to ignore Greer, doing anything he wants on a whim to screw with trade and the entire global market without accountability.
Not to mention dicking around with showerheads.
One might wonder when the GOP members of Congress will organize and get a collective spine and consider impeaching and convicting a president who thinks government is just his personal chew toy, treating Congress like they’re irrelevant.
How many angry constituents will it take before they catch a clue? Are they really more afraid of a guy obsessed with showerheads than their own voters?
~ ~ ~
Speaking of angry constituents, please recruit others to help combat H.R. 22, the voter suppression bill Republicans call the SAVE Act. Contact every person you know and ask them to contact their representatives and ask them to vote down this bill.
See: https://indivisible.org/campaign/trumps-new-executive-order-eo-silence-americans-what-you-need-know
As our team member Peterr wrote in comments yesterday,
While it is critical to call your GOP representatives to let them know how much you are opposed to this un-American bill, it is at least as important to call your Democratic reps to tell them to stand up to this, and thank them for doing so.
As a pastor, I am quite familiar with getting phone calls from folks who dislike something I believe needs to be done. Getting the “thank you” calls makes it a lot easier to do what I believe needs to be done. This is how you help Dems grow a stronger spine.
Call your representative no matter their party affiliation. This is too important, leave no stone unturned. When you’re done, call your senators and ask them not to support the SAVE Act just as you did your representative.
If you’re a member of a women’s group, recruit them all because women are the largest single bloc likely to be disenfranchised by this bill.
Don’t wait, make this a priority because a vote could happen as early as today.
~ ~ ~
UPDATE – 8:30 PM ET —
H.R. 22 passed the House nearly along party lines, 220-208.
Four Democrats voted along with the GOP to disenfranchise a substantive portion of their own constituents let alone their own voters. Apparently they don’t care if they ever win election again.
Indivisible emailed an update; if you’re on their mailing list you may also have been told how your representative voted. Of course those of you who are represented by these four Democrats have been betrayed:
Ed Case (HI-01)
Henry Cuellar (TX-28)
Marie Gluesenkamp Perez (WA-03)
Jared Golden (ME-02)
Our next step is to contact your senators and ask them to vote down the SAVE Act.
The Senate only is in session tomorrow (H.R. 22 was one of the last pieces of business on which the House GOP scheduled a vote before fleeing Washington DC). Congress will be on holiday break and in a state work session from April 12 through April 27.
Contact your senators’ closest local office and find out if they are having town halls or will be at other events where you can ask them in person to vote against the SAVE Act.
VoteVets has also sent out an email about the damage this bill poses to the rights of military personnel:
Trump and Elon’s agenda is overwhelmingly unpopular. We’ve got the GOP on their heels.
And now — like clockwork — Republicans are desperate to make it harder for people to vote.
Republicans in the House passed the SAVE Act today, under the guise of election security. It’s a blatant effort to make it harder for people to register to vote and cast their ballot. And if it becomes law, it’s going to impact Veterans, Military Families, and Active Duty.
SAVE would require all voters, including Military voters, to present very specific proof of US citizenship — either a passport or a birth certificate — in person at a government office in the United States to register or update their voter registration. Military IDs and service records are not enough proof to register. It would ban automatic, online, and mail in registration.
How might all of that impact Troops deployed overseas, their spouses, or disabled Veterans who can’t get to an office? It could effectively ban them from registering.
This bill is terrible. It’s an effort to suppress Military votes. If it passes the Senate, it’s going to undermine our elections. And today, we need you to speak out against it.
I hope VoteVets has a chat with veteran Jared Golden over his betrayal of veterans, military families, and active duty service members.
There’s one more important reason this bill needs to be defeated, besides the fact it will disenfranchise a massive number of American voters.
We voters can’t save Republicans from themselves and their leader if we can’t vote. Some of the GOP senators *know* everything is going to hell in a handbasket. They own it if there isn’t a brake applied. This is one of those brakes — they can vote to preserve their constituents’ right to vote by voting against the SAVE Act.
If you can’t find your senators’ local office numbers, you can always contact them through the Congressional switchboard at (202) 224-3121, or use Resist.bot to contact them.
Don’t sit this one out, it’s far too big, far too important. It’s especially important to contact these Democratic senators if you live in their states because their track record isn’t good based on their previous votes related to immigration:
Catherine Cortez Masto (NV)
John Fetterman (PA)
Ruben Gallego (AZ)
Maggie Hassan (NH)
Mark Kelly (AZ)
John Ossoff (GA)
Gary Peters (MI)
Jacky Rosen (NV)
Jeanne Shaheen (NH)
Elissa Slotkin (MI)
Mark Warner (VA)
Raphael Warnock (GA)
I’m embarrassed to say two of them are my senators. I will be contacting them, though. I can’t afford not to. And I will recruit others to do so, too.
Get them on the record as soon as you can, too. Where do they stand? Let’s keep track.