This post is in two parts. The first part deals with the news that a new flu virus has emerged. The second part, which comes below the fold, provides a bit of biological and public health information to help put the news into perspective.
According to the latest reports I can find, there are now three confirmed deaths and ten confirmed cases of people infected with a new strain of Type A (bird) influenza virus that has been designated H7N9. All cases have been in eastern China. The good news is that there is not yet evidence to suggest that this virus can spread from one person to another (although that question has not yet been fully answered), which is a prerequisite for a pandemic. The bad news, though, is that the animal host from which the infections were acquired has not been identified.
Earlier this week, Laurie Garrett began assembling what is known about the emerging cases of H7N9 infection and putting those cases into the context of mysterious mass die-offs of pigs and birds in the same general region of China (Garrett is asking important questions here since previous flu pandemics have come from swine or bird hosts):
By the end of March, at least 20,000 pig carcasses and tens of thousands of ducks and swans had washed upon riverbanks that stretch from the Lake Qinghai area all the way to the East China Sea — a distance roughly equivalent to the span between Miami and Boston. Nobody knows how many more thousands of birds and pigs have died, but gone uncounted as farmers buried or burned the carcasses to avoid reprimands from authorities.
While environmental clean-up and agricultural authorities scrambled to remove the unsightly corpses and provide the anxious public with less-than-believable explanations for their demise, a seemingly separate human drama was unfolding. On Feb. 19, a man identified by Xinhua, China’s state news agency, only as Li, an 87-year old retiree, was hospitalized in Shanghai with severe respiratory distress and pneumonia. On March 4, Li went into severe cardio-respiratory failure and succumbed.
On Feb. 27, a man identified only as Wu, a 27-year-old butcher or meat processor, fell ill with respiratory distress, was hospitalized, and died on March 10. The day Wu succumbed a third individual, a 35-year-old woman identified as Han, was hospitalized in the city of Nanjing, though she came from distant Chuzhou City, in Anhui province, about 300 miles northwest of Shanghai. Han is reportedly in critical condition, in intensive care. To date, no connection between the three individuals has been found.
The key question of whether person-to-person transmission of the virus can occur is made somewhat murky by the family of Li:
The elderly Li may have been part of a family cluster of illness, as his 55-year old son died of pneumonia in March, and another 67-year-old son suffered respiratory distress, but has survived.
On March 31 — Easter in the United States — China’s newly created National Health and Family Planning Commission (which includes the former Ministry of Health) announced that 87-year-old Li, Wu, and Han all were infected with a form of influenza denoted as H7N9 — a type of flu never previously known to infect human beings. The commission insisted that Li’s two sons (one dead, the other a survivor) were not infected with the flu virus — their ailments were reportedly coincidental, though they occurred at the same time as the elder Li’s demise.
Garrett goes on to point out that Chinese authorities have blamed a non-influenza virus for the pig deaths, but she casts some doubt on this claim, since the virus cited by the Chinese is known to kill young piglets but not adult pigs. The dead pigs found tossed into rivers primarily were adults.
Garrett rightly states that our knowledge of what is going on here is highly dependent on the accuracy of the tests that authorities are carrying out:
If the pigs, people, and birds have died in China from H7N9, it is imperative and urgent that the biological connection be made, and extensive research be done to determine how widespread human infection may be. Shanghai health authorities have tested dozens of people known to have been in contact with Wu and Li, none of whom have come up positive for H7N9 infection. Assuming the tests are accurate, the mystery of Li and Wu’s infections only deepens. Moreover, if they are a “two of three,” meaning two dead, of three known cases, the H7N9 virus is very virulent.
“At this point, these three are isolated cases with no evidence of human-to-human transmission”, the WHO representative in China, Dr. Michael O’Leary, told reporters on Monday. But, O’Leary added, the possibility of a family cluster of illness could not be ruled out, and, “We don’t know yet the causes of illness in the two sons, but naturally, if three people in one family acquire severe pneumonia in a short period of time, it raises a lot of concern.”
The key phrase above is “Assuming these tests are accurate”. When a new virus emerges, it is difficult to know what tests to conduct to detect the virus and how to conduct those tests. More detail is clearly needed to know what level of confidence can be placed on the Chinese claim that Li’s family members were not infected with the same virus that killed him.
Garrett puts these questions into more context in the Reuters article linked above:
However, China has yet to find any animals infected with H7N9, meaning how the humans got it remains a mystery.
“We know that it was originally a bird virus. We also know that it has taken on some genetic attributes that are not seen in bird viruses,” Laurie Garrett, Senior Fellow for Global Health at the Council for Foreign Relations, told Reuters in New York.
“In other words, it seems to have adapted somehow to mammals, to humans. How that happened, we don’t know,” added Garrett.
Update: Via Twitter, Laurie Garrett points out that Chinese authorities now have evidence that pigeons in Shanghai have been infected with a version of the H7N9 virus that is a genetic match to the viruses isolated from humans, so pigeons may be the source. More can be read here.
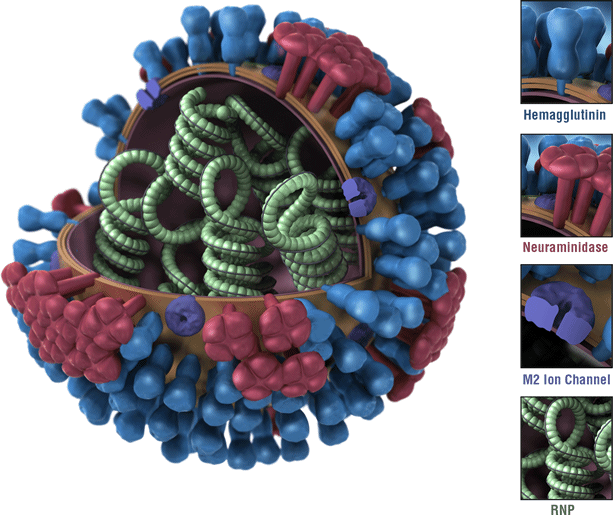
The schematic above (provided by CDC) shows the structure of an influenza virus particle. There are two major proteins found on the virus surface, hemagglutinin (that is the “H” when the virus type is designated) and neuraminidase (the “N”). Infection of humans occurs primarily through breathing in small droplets of aerosolized virus particles. The hemagglutinin is responsible for the virus binding to specific structures on cells lining the respiratory tract. Once binding to the receptor occurs, the virus outer membrane merges with the cell membrane. The virus carries only eight small genes. The genetic information in flu viruses is present as RNA rather than DNA. The viral RNA moves to the cell nucleus, where it makes many copies of itself. Some of that RNA is converted to messenger RNA that hijacks the cell’s protein-making machinery to make new proteins that assemble with the new viral RNA to make new virus particles.
The neuramindase is important to the process of the new viral particles budding off from the host cell. Inhibitors of neuraminidase, such as Tamiflu, interrupt this process and can make a person’s flu infection much less severe, but only if administered in the early stages before the infection has spread widely from the first few infected cells. Flu vaccines work by stimulating the production of antibodies against the the surface features of a virus (such as the hemagglutinin and neuraminidase), but protection is afforded only to those viruses which are used to produce the particular vaccine. This year’s flu vaccine did not include H7N9 and is unlikely to provide protection from it.
The World Health Organization has produced a very informative set of FAQ regarding the H7N9 outbreak. Given the widespread pig and bird deaths in China, this question is especially helpful:
9. Is it safe to eat meat, i.e. poultry and pork products?
Although we do not yet know the mode of transmission, it is prudent to follow basic principles of hygienic food preparation, as follows: Diseased animals should not be eaten. Otherwise, it is safe to eat properly prepared and cooked meat. Because influenza viruses are inactivated by sufficient heating, normal temperatures used for cooking (such that food reaches 70°C in all parts— “piping” hot — no “pink” parts) will kill the virus. In areas experiencing outbreaks, meat products can be safely consumed provided that these items are properly cooked and properly handled during food preparation. The consumption of raw meat and uncooked blood-based dishes is a high-risk practice and is discouraged. Always keep raw meat separate from cooked or ready-to-eat foods to avoid contamination. Do not use the same chopping board or the same knife for raw meat and other foods. Do not handle both raw and cooked foods without washing your hands in between and do not place cooked meat back on the same plate or surface it was on before cooking. Do not use raw or soft-boiled eggs in food preparations that will not be heat treated or cooked. After handling raw meat, wash your hands thoroughly with soap and water. Wash and disinfect all surfaces and utensils that have been in contact with raw meat.
General advice for protecting against infection also is provided:
8. How can infection with influenza A(H7N9) virus be prevented?
Although both the source of infection and the mode of transmission are uncertain, it is prudent to follow basic hygienic practices to prevent infection. They include hand and respiratory hygiene and food safety measures.
Hand hygiene:
• Wash your hands before, during, and after you prepare food; before you eat; after you use the toilet; after handling animals or animal waste; when your hands are dirty; and when providing care when someone in your home is sick. Hand hygiene will also prevent the transmission of infections to yourself (from touching contaminated surfaces) and in hospitals to patients, health care workers and others.
• Wash your hands with soap and running water when visibly dirty; if not visibly dirty, wash your hands with soap and water or use an alcohol-based hand cleanser.Respiratory hygiene:
• Cover your mouth and nose with a medical mask, tissue, or a sleeve or flexed elbow when coughing or sneezing; throw the used tissue into a closed bin immediately after use; perform hand hygiene after contact with respiratory secretions.
WHO also is providing alerts on the emergence of H7N9. The latest can be read here and new ones should be accessible from this page.